For 34 years, my academic and clinical interests have primarily centered around whiplash trauma, its understanding and management. I have often heard that the pathology for both acute and chronic whiplash pain are unknown and undiagnosable. It is commonplace to label the pathology of whiplash syndrome as unknown, self limiting, psychometric, secondary gain, biosocial, etc. However, all of this is largely not true.
Perhaps, the most accomplished clinical anatomist of our time is Nikolai Bogduk, MD, PhD, from Australia. Dr. Bogduk is a professor of Pain Medicine at the University of Newcastle and the Head of the Department of Clinical Research at the Royal Newcastle Hospital in Newcastle, Australia. He was the Director of the National Musculoskeletal Medicine Initiative in Australia (from 1997 to 2001) and is currently a member on the Executive Group of the Guidelines for Acute Musculoskeletal Pain in Australia. Dr. Bogduk is on the Editorial Board for many publications including Spine, The Spine Journal, Clinical Biomechanics, Pain Medicine and Cephalalgia.
Dr. Bogduk began researching the anatomical basis of various spinal syndromes 40 years ago (1972). A PubMed search of the National Library of Medicine using “bogduk n” brings up 216 citations (January 10, 2012). Dr. Bogduk has authored 9 books on various aspects of clinical anatomy (the most recent being this year, 2012), and many chapters in others books. Dr. Bogduk has been the single most published person in history on the anatomical basis of acute and chronic whiplash pain syndrome.
The understanding of whiplash biomechanics was forever changed when an experimental study appeared in the journal Spine in November 1997 (1). In this study, Grauer and associates from the Department of Orthopaedics and Rehabilitation at Yale University School of Medicine performed a series of rear-end collisions on human cadavers. Because the subjects in this series were cadavers, exposure to ionizing radiation was moot, allowing the team to view cervical spine dynamics during the collision using cineradiography. This unique method of assessment brought forth the following conclusions and opinions:
- In the earliest phase of the cervical spine dynamics following a rear-end collision, the cervical spine forms an “S” shaped configuration, with flexion of the upper cervical spine and simultaneous significant hyperextension of the lower cervical spine.
- The tissue distortion noted during this “S” configuration of the cervical spine was of a magnitude that is injurious.
- This injurious “S” configuration of the cervical spine occurs very quickly, between 50 – 75 milliseconds following impact.
- The quickness of this “S” configuration of the cervical spine is shorter than the time required by the stretched muscles to react and to afford meaningful protection of the cervical spine joints. Therefore, the injury is primarily imparted to the joints of the cervical spine.
- In most cases, this quick injurious “S” configuration of the cervical spine occurs before the head contacts the head restraint, meaning the head restraint often does not offer adequate protection.
Several other cadaver studies confirmed this “S” configuration of the cervical spine in the initial phase of whiplash injury. In 1999, similar cineradiography studies were performed on live human volunteers by Kaneoka and colleagues (2), and the results were the same as those of the cadaver studies. This 1999 live human volunteer study generated this following official (invited) Point of View, published in Spine:
POINT OF VIEW
Nikolai Bogduk, MD, PhD, DSc, FAFRM
Department of Anatomy and Musculoskeletal Medicine
University of Newcastle
Newcastle Bone and Joint Institute
Royal Newcastle Hospital
Newcastle, New South Wales, Australia
“The study of Kaneoka et al now fills a critical gap in the story of cervical facet pain. It provides the missing biomechanical link. Their’s is the most significant advance in the biomechanics of whiplash since the pioneering studies of Severy et al in 1955.”
“As a result of this study, we no longer rely on inference or speculation; we have a direct demonstration of the mechanism of injury in whiplash.”
Essentially all articles published regarding whiplash biomechanics since 1997 – 1999 cite these studies that agree the pathology of whiplash primarily occurs during this “S” configuration very early on (50–75 ms) following the collision. As an example, last fall (October 2007), a review article by Schofferman and colleagues (3) titled:
Chronic whiplash and whiplash-associated disorders:
An evidence-based approach
Journal of the American Academy of Orthopedic Surgeons
October 2007;15(10):596-606
makes the following comments:
“In a typical rear-end motor vehicle collision, the injury is caused by the abnormal biomechanics of neck motion resulting from the forward and upward motion of the torso while the head lags behind as the result of inertia.”
“Whiplash injury is any structural damage sustained because of the whiplash forces.”
“The forward acceleration of the torso deforms the cervical spine into a nonphysiologic S-shaped curve, with extension developing between the lower segments and flexion developing between the uppermost segments. Most of the whiplash injury occurs during this deformation phase.”
“The cervical facet joint is the most common source of chronic neck pain after whiplash injury, followed by disk pain. Some patients experience pain from both structures.”
“The facet joints are the most common source [more than half of the cases] of chronic neck pain after whiplash injury.”
“Some patients have pain that arises from a disk, and some have a combination of facet joint pain and discogenic pain.”
•••••••••
Importantly, the 1999 live human cineradiography cervical spine biomechanical study by Kaneoka and colleagues (2) showed that the primary injury from whiplash trauma was to the facet joints and to the intervertebral disc. Their article makes the following points:
“The zygapophysial joint is the suspected origin of neck pain after rear-end car collision.”
The facet joint collision that occurs during the first phase of whiplash trauma creates a bending moment. “If this bending moment is large enough, this motion is likely to cause the disruption of the disc from the vertebral rim (rim lesion) or to cause a zygapophysial joint injury.”
“Most whiplash injuries occur during low-speed rear-end collisions and rarely produce morphologic changes such as fracture of the joint. The zygapophysial joint is a synovial joint and has a synovial fold (meniscus), between the articular facets that is innervated with nociceptive receptors. Thus, we hypothesize that facet collisions are likely to impinge on and inflame the synovial folds in the zygapophysial joints, causing neck pain (facet synovial fold impingement syndrome).”
Once again, in the official, invited POINT OF VIEW by Dr. Bogduk of the Kaneoka study, the following comments are found:
“The critical observation is that in whiplash the lower cervical segments undergo sagittal rotation about an abnormally high instantaneous axis of rotation. As a result, there is no translation; there is only rotation. As the vertebra spins, its anterior elements separate from, while the posterior elements crunch into, the vertebra below. This mechanism predicts that the resultant lesions should be tears of the anterior annulus and fractures of the zygapophysial joints or contusions of their meniscoids. These are the very lesions seen at postmortem.”
In 2002, additional evidence for whiplash trauma causing injury to the facet joints and intervertebral disc of the lower cervical spine was presented by Lars Uhrenholt and colleagues from the Institute of Sports Science and Clinical Biomechanics, University of Southern Denmark, Odense, Denmark (4). Their study, published in Spine, was titled:
Cervical spine lesions after road traffic accidents:
a systematic review
The authors concluded that occult pathoanatomical lesions in the cervical intervertebral disc and zygapophysial joints were possible in survivors of motor vehicle collisions. This article was also well summarized in the Point Of View from Dr. Nikoli Bogduk, as follows:
Point of View
Nikolai Bogduk, MD
This study has “harvested the best available evidence concerning the possible pathology of whiplash.”
The injuries documented include:
(1) Articular fractures
(2) Intra-articular contusions
(3) Tears of the anterior annulus
The credibility of these injuries is enhanced because different lines of investigation, using totally independent methods, point to the same conclusion. “This constitutes convergent validity.”
“In the case of whiplash, postmortem studies, biomechanics studies, and clinical studies converge.”
“Postmortem studies point to lesions in the zygapophysial joints.”
“Biomechanical studies show how these joints can be injured to produce the lesions seen at mortem.”
“Clinical studies have shown that zygapophysial joint pain is common in patients with chronic neck pain after whiplash.”
“All three lines of investigation point to the same culprit,” the facet joint.
Two years later, in 2004, Pearson and colleagues from the Biomechanics Research Laboratory, Department of Orthopaedics and Rehabilitation, Yale University School of Medicine, published in the journal Spine the most detailed evidence to date showing the biomechanics of facet joint injury during whiplash mechanism (5). Their article is titled:
Facet joint kinematics and injury mechanisms during simulated whiplash
•••••••••
In 1993, Drs. Nikoli Bogduk and Charles Aprill published primary research in the journal Pain (6) pertaining to the sources of chronic neck pain by using both provocation discography and cervical zygapophysial joint blocks. Comments found in their study include:
“Both a symptomatic disc and a symptomatic zygapophysial joint were identified in the same segment in 41% of the patients.”
“Discs alone were symptomatic in only 20% of the sample.”
“Zygapophysial joints were symptomatic but discs were asymptomatic in 23%.”
“Only 17% of the patients had neither a symptomatic disc nor a symptomatic zygapophysial joint at the segments studied.”
Neck muscle injury “does not provide a satisfying model for persistent or chronic neck pain” because extremity muscle injuries heal rapidly, “in a matter of days or weeks.”
Persistent neck pain suggests injury to tissues that heal poorly or slowly, such as the intervertebral disc and the facet joints. “However, painful disorders of these structures are not demonstrable by plain radiography, computed tomography or magnetic resonance images.”
No findings on plain radiography, computed tomography or magnetic resonance images are correlated with pain.
The most frequent finding was “both a symptomatic disc and a symptomatic zygapophysial joint at the same segment,” seen in 41%.
The second most frequent finding was a symptomatic zygapophysial joint, alone, with no disc involvement, which was found in 23%.
“This indicated that 64% of the sample had a symptomatic zygapophysial joint.” [41% + 23% = 64%]
The third most frequent finding was a symptomatic disc alone, with no zygapophysial joint involvement, found at 20%.
This indicated that 61% of the sample had a symptomatic disc.
[41% + 20% = 61%]
“If cervical segments are fully investigated, it emerges that cervical discs are not the most common, primary source of neck pain.”
“A large proportion, if not the majority, of patients with post-traumatic neck pain have symptomatic zygapophysial joints.”
•••••••••
In the following few years, Dr. Bogduk ad colleagues continued to engage in primary research pertaining to the clinical sources of chronic whiplash pain. In 1995, they published a study in the journal Spine titled (7):
The prevalence of chronic cervical zygapophysial joint pain after whiplash
In this study, the authors note and conclude:
“In a significant proportion of patients with whiplash, chronic, refractory neck pain develops.”
“Painful joints were identified in 54% of the patients.”
“In this population, cervical zygapophysial joint pain was the most common source of chronic neck pain after whiplash.”
The following year in 1996 the same authors publish a follow-up article in Spine titled (8):
Chronic cervical zygapophysial joint pain after whiplash:
A placebo-controlled prevalence study
Their findings and conclusions include:
“Overall, the prevalence of cervical zygapophysial joint pain (C2-C3 or below) was 60%.”
“Cervical zygapophysial joint pain is common among patients with chronic neck pain after whiplash.”
•••••••••
The entire December 1, 2011 supplement of the journal Spine is dedicated to whiplash trauma. The issue contains 27 articles by the world’s foremost authorities on whiplash biomechanics, pathology and outcomes. Importantly, and as appropriately expected, Dr. Bogduk is a co-author for two of the articles and a solo author for one study. Dr. Bogduk’s solo article pertains to the facet joint, and is titled (9):
On Cervical Zygapophysial Joint Pain After Whiplash
In this article, Dr. Bogduk cites 72 references while summarizing the evidence that implicates the cervical zygapophysial joints as the leading source of chronic neck pain after whiplash trauma. He states that the patho-anatomic basis for neck pain after whiplash is not elusive, but rather well documented and well known. Dr. Bogduk notes that there is convergent validity from (1) whiplash postmortem studies, (2) whiplash biomechanics studies, and (3) whiplash clinical studies indicating that the primary source of chronic whiplash pain is injury to the cervical zygapophysial joints. He sumarizes by noting that in whiplash, four convergent lines of evidence “implicate the cervical zygapophysial joints as the leading source of pain in patients with chronic whiplash-associated disorder:”
- Postmortem studies show that a spectrum of injuries occur in the facet joints in motor vehicle accidents.
- Biomechanics studies of normal volunteers and of cadavers reveal the mechanisms by which the facet joints sustain injury during whiplash.
- Whiplash studies in cadavers and laboratory animals have produced facet joints injuries.
- Clinical studies have shown that facet joint pain is very common among patients with chronic neck pain after whiplash.
•••••••••
The postmortem studies identified a variety of nonlethal injuries:
- Nerve-root lesions
- Rim-lesions to the intervertebral discs (the disc is traumatically separated from the cartilaginous end-plate of the vertebral body)
- Intraarticular hemorrhages
- Fractures of the facet articular cartilage
- Fractures of the facet subchondral bone
- Fractures of the entire facet articular processes
Importantly, virtually none of these lesions were seen on postmortem radiography. Dr. Bogduk states:
“Medical imaging in vivo may fail to identify lesions that are definitely present at postmortem. Consequently, in the context of whiplash injury, normal radiographs, or even normal magnetic resonance imaging, do not mean that the patient has no lesion.”
•••••••••
The human biomechanics studies identified these injurious mechanisms:
- The cervical spine undergoes a “highly abnormal” “S” shaped deformation with extension of the lower cervical spine and flexion of the upper cervical spine.
- During the extension of the lower cervical spine, the anterior margins of the vertebral bodies are widely separated, resulting in an avulsion of the annulus fibrosus from the vertebral endplate (a rim lesion).
- Also during the extension of the lower cervical spine the inferior facet articular process chisels into the superior facet articular surface of the vertebra below, allowing for a spectrum of lesions to the facet joints.
- The intraarticular meniscoids could be contused or ruptured
- Impaction fractures of the articular processes could occur
- Cadaver studies during whiplash show that the facet joints undergo compression that exceeds physiological limits and the capsules undergo strains beyond normal limits.
- Strains in the annulus fibrosus can exceed normal limits.
Dr. Bogduk states:
“Collectively, these various biomechanics studies, in normal volunteers and in cadavers, predict or produce the same spectrum of lesions as that identified in postmortem studies. In particular, they indicate that the zygapophysial joints can be injured.”
Dr. Bogduk lists the following proven non-lethal pain producing injuries caused by whiplash trauma
- Intra-articular Hemorrhage [causes organization, adhesions, fibrosis]
- Facet Capsular Tear
- Meniscoid Contusion [can result in joint motion block, spasm, torticollis]
- Articular Subchondral Fracture [acceleration of cartilage arthritis]
- Fracture of the Articular Pillar
- Disc Tear or Torn From the Vertebral Rim [acceleration of disc degenerative disease, these injuries do not heal (reattach)]
Overall, Dr. Bogduk indicates that the prevalence of neck pain stemming from a facet joint is just over 50%, indicating the facet joint is a very common source for neck pain. Dr. Bodguk cites 7 studies showing a prevalence of cervical facet joint pain between 36-67%.
| Year | Journal | Prevalence |
| 1995 | Spine | 54% |
| 1996 | Spine | 60% |
| 2001 | Medical Journal of Australia | 36% |
| 2002 | Pain Physician | 67% |
| 2007 | Journal of Spinal Disorders and Techniques | 39% |
| 2008 | Pain Medicine | 46% |
| 2008 | Pain Physician | 39% |
Dr. Bogduk concludes:
“The zygapophysial joints are the single, most common source of pain in patients with chronic neck pain after whiplash.”
There is an extensive amount of evidence indicating that post-whiplash pain syndrome is attributed to injury to the cervical facet joints; no other explanation for whiplash pain has more evidence.
•••••••••
Dr. Bogduk notes that chronic cervical facet joint pain can be treated with radiofrequency neurotomy (the ablation of the nerves that transmit pain from the injured facet joints). However, he also qualifies the statement with:
- Radiofrequency Neurotomy only treats cervical facet pain, which afflicts about 50% of those suffering from chronic whiplash pain. The other 50% of chronic whiplash pain sufferers are not amenable to the Radiofrequency Neurotomy procedure.
- Inclusion criteria for the Radiofrequency Neurotomy procedure requires successful pain relief with diagnostic blocks of the medial branch of the posterior primary rami performed on two separate occasions.
- Successful Radiofrequency Neurotomy on appropriately selected patients is about 70%, and the pain relief lasts for a medium of about 400 days. This would mean that the procedure works on about 35% of chronic whiplash patients [50% X .7 = 35%] for about 400 days on average. Dr. Bogduk notes that if/when the pain returns, the procedure can be repeated.
- “Medial branch blocks and radiofrequency neurotomy cannot be performed other than by specially trained, medical practitioners,” and there are very few medical practitioners who are properly trained and qualified to do these procedures. He states:“Few practitioners around the world are skilled in these procedures; and among those who purport to be skilled, there is no guarantee that they perform the procedures properly.” “The available evidence indicates that good outcomes can only be expected if those guidelines are followed.”
- Some medical practitioners that claim do to these procedures do not follow the proper guidelines, performing it “irresponsibly if not fraudulently.”
- Radiofrequency neurotomy outcomes in patients pursuing litigation are about the same as in patients not involved in litigation.
Whiplash Injury Facet Pain
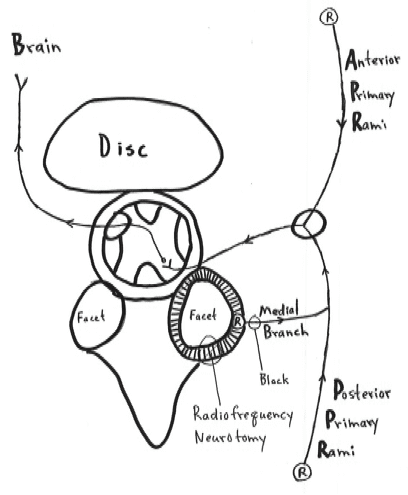
Whiplash injures the facet joint.
The facet joint has nociceptors “R” which are connected to the brain through the medial branches of the posterior primary rami.
If diagnostic anesthetic blocking of the medial branch of the posterior primary rami eliminates pain, it indicates the facet is the source of the pain.
Radiofrequency neurotomy of the facet joint capsules coagulates the neurofiliment proteins, giving 70% of the patients longer relief of their whiplash pain.
This study by Dr. Bogduk reiterates:
- Many involved in a whiplash injury develop chronic neck pain.
- This chronic whiplash-generated neck pain does not seem to be associated with litigation status.
- The primary injury and source of pain in the chronic whiplash patient is the facet joint.
- It is highly unlikely that the pain producing facet joint injury, including fractures, are discernable with either radiography or MR imaging.
- For facet joint pain to be definitely ruled-in or ruled-out, the patient must undergo, on two separate occasions, medial branch blocks of the posterior primary rami.
Although Dr. Bogduk is advocating radiofrequency neurotomy ablation of the facet joint nerves as the best treatment option in the management of chronic whiplash pain, it should be understood that:
- only about 50% of chronic whiplash patients are appropriate for this procedure
- it only works on about 70% of those judged to be appropriate candidates for the technique, and
- the effective pain relief is for about 400 days
Chiropractic adjusting affects many tissues but primarily the facet joints. There are several studies indicating that chiropractic spinal adjusting is more effective that radiofrequency neurotomy ablation in the treatment of the chronic whiplash patient (10, 11). The Woodward study was 93% effective (10). The Khan study was 74% effective (11). We have reviewed both studies several times before. Consequently, I believe that chiropractic spinal adjusting should be performed on all chronic whiplash patients prior to having the patient undergo medial branch blocks of the posterior primary rami and radiofrequency neurotomy ablation of the facet joints.
OTHER CONCERNS
Radiofrequency ablation of the facet joints not only stops nociception but also stops mechanoreception. Many chiropractors, including myself, and other providers, are concerned that ablation of the mechanoreceptors may adversely affect local neuromuscular reflexes controlling stability and therefore the incidence of future joint degeneration, as well as adversely affecting central summation and central neurological function. These concerns could have critical long-term implications for whiplash patients treated with radiofrequency neurotomy. Consequently, I reiterate that radiofrequency neurotomy should only be performed if Chiropractic and other conservative approaches have not delivered acceptable clinical outcomes.
•••••••••
References:
1) Grauer JN, Panjabi MM, Cholewicki J, Nibu K, Dvorak J. Whiplash produces an S-shaped curvature of the neck with hyperextension at lower levels. Spine. 1997 Nov 1;22(21):2489-94.
2) Kaneoka K, Ono K, Inami S, Hayashi K. Motion analysis of cervical vertebrae during whiplash loading. Spine. 1999 Apr 15;24(8):763-9.
3) Schofferman J, Bogduk N, Slosar P. Chronic whiplash and whiplash-associated disorders: An evidence-based approach; Journal of the American Academy of Orthopedic Surgeons; October 2007;15(10):596-606.
4) Uhrenholt L, Grunnet-Nilsson N, Hartvigsen J. Spine. Cervical spine lesions after road traffic accidents: a systematic review; 2002 Sep 1;27(17):1934-41.
5) Pearson AM, Ivancic PC, Ito S, Panjabi MM. Facet joint kinematics and injury mechanisms during simulated whiplash; Spine; 2004 Feb. 15; 29(4):390-7.
6) Bogduk N, Aprill C. On the nature of neck pain, discography and cervical zygapophysial joint blocks; Pain; August 1993;54(2):213-7.
7) Barnsley L, Lord SM, Wallis BJ, Bogduk N. The prevalence of chronic cervical zygapophysial joint pain after whiplash. Spine. 1995 Jan 1;20(1):20-5.
8) Lord SM, Barnsley L, Wallis BJ, Bogduk N. Chronic cervical zygapophysial joint pain after whiplash. A placebo-controlled prevalence study. Spine. 1996 Aug 1;21(15):1737-44.
9) Bogduk N; On Cervical Zygapophysial Joint Pain After Whiplash; Spine
December 1, 2011; Volume 36, Number 25S, pp S194–S199.
10) Woodward MN, Cook JCH, Gargan MF, and Bannister GC. Chiropractic treatment of chronic ‘whiplash’ injuries; Injury; Volume 27, Issue 9, November 1996, pp 643-645.
11) Khan S, Cook J, Gargan M, Bannister G. A symptomatic classification of whiplash injury and the implications for treatment; The Journal of Orthopaedic Medicine 21(1) 1999, 22-25.
