When examining a patient for hip pain and other musculoskeletal conditions, doctors of chiropractic will expand their focus beyond the area of chief complaint to identify issues elsewhere in the body that may be underlying or contributing factors. This is especially true with the hip because anything that affects normal locomotion can lead to compensatory changes and abnormal motion in the hip joint, which can easily result in inflammation or wear and tear that causes pain. Such is the case with issues in the foot, like plantar fasciitis.
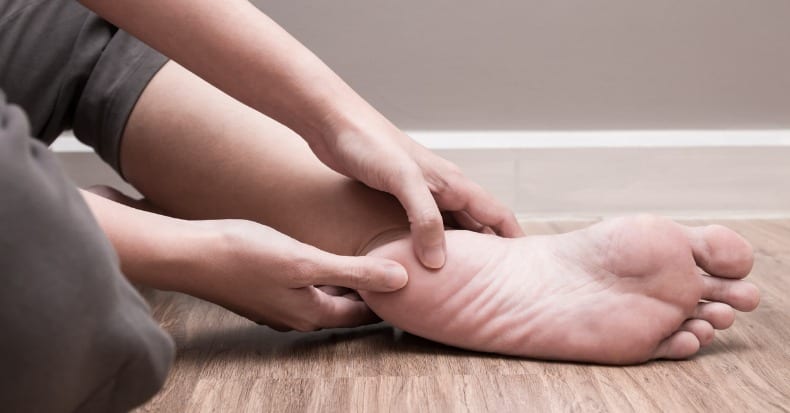
Plantar fasciitis is one of the most common causes of heel pain and is characterized by inflammation of the thick band of tissue (plantar fascia) located on the bottom of the foot that connects the heel bone (calcaneus) to the toes. Individuals with the condition may experience a stabbing pain that often occurs with initial weightbearing, especially in the morning. The intense initial pain usually improves after a few steps; however, it can also worsen following prolonged standing or intense activity.
The function of the medial longitudinal arch of the foot is to absorb shock and to add “spring” to each step. In the mid-stance phase of gait, the arch flattens out, stretching the plantar fascia (the “string”) and if stress and tension exceeds the tissue’s threshold or becomes too great, micro-tears inflame the fascia and cause pain when initiating weightbearing. This leads to pain and can affect normal gait, which can ultimately lead to issues up the kinetic chain, such as hip pain.
Risk factors for PF include advancing age, stressful exercise (running, ballet dancing, aerobic dance), altered arches in the feet (such as flat feet as well as a high arch), obesity, and occupations that require an individual to be on their feet all day, especially on hard surfaces.
Following diagnosis, which may include a review of the patient history and an examination, a conservative treatment approach in a chiropractic setting may include manual therapies (longitudinal and cross fiber friction massage); Graston technique (using spoon-like tools to stimulate blood flow and break up adhesions); stretching exercises (calf stretches off a step or using TheraBand to bend the foot and ankle upwards and extend the toes); prescription foot orthotics with pronation correction (lateral heel wedge); modalities (laser, ultrasound, extracorporeal shock wave therapy); and dorsiflexion night splinting. Patients may also be encouraged to reduce their intake of processed foods—which can increase inflammation in the body—and eat a more anti-inflammatory diet, like the Mediterranean diet, to aid in the healing process.
Because prolonged standing and stressful exercise can worsen the condition, patients may be advised to reduce the time they spend on their feet and switch to less impactful forms of exercise during recovery.
The good news is that conservative treatment approaches, such as chiropractic care, are often successful in helping PF patients manage their condition.